How a Canadian Dental Clinic Should Budget Cybersecurity
The biggest cybersecurity mistake for most small clinics is allocating their budget poorly. Many clinics either underestimate the budget required because they assume they are too small to be targeted, or they overreact after an incident by buying tools in a hurry without any underlying architecture. Neither approach is strategic.
Matthieu Chouinard
3/29/202610 min read


The budgeting problem most clinics solve too late
A dental clinic does not experience cybersecurity as an abstract technology problem. It experiences it as cancelled appointments, inaccessible charts and imaging, front-desk chaos, delayed claims, anxious patients, and difficult privacy conversations with regulators. In other words, cyber risk manifests as operational stoppages, employee stress, increased insurance premiums, fines, legal fees, system recovery costs, and investigations.
“Responding to an attack may require hiring experts like forensic investigators, lawyers and public relations professionals, which can be extremely costly for businesses that don’t have dedicated cyber insurance. A stand-alone cyber policy can also help cover costs associated with lost income, recovery efforts and legal liabilities,” said Mahan Azimi, Director, Catastrophic and Emerging Risk Policy, IBC.
That is why budgeting cybersecurity badly is so expensive. Many clinics either under-budget because they assume they are too small to be targeted, or they overreact after an incident by buying tools in a hurry with no clear vision behind them. Neither approach is strategic. The real task is simpler: define what must keep working, estimate what interruption would cost, and fund the minimum set of controls that meaningfully reduces that risk.
Real-world insurance data paints a far more concrete and alarming picture for small- and mid-sized businesses. According to the 2025 NetDiligence Cyber Claims Study, the average cost of a cyber incident for SMEs is now approximately $246,000 to $264,000, with costs rising nearly 30% year over year. Ransomware and business email compromise remain the dominant causes of loss, accounting for most claims and financial impact. Furthermore, the data shows that when business interruption is involved, total incident costs can increase by more than 650%. This makes operational downtime, rather than just data loss, the primary driver of financial damage.
Beyond averages, severity continues to escalate. Ransomware incidents alone can exceed $600,000 on average for SMEs, while overall five-year average incident costs approach $937,000 when all recovery, legal, and operational impacts are included.
For small businesses, this creates what analysts describe as an “insolvency gap”: typical cash reserves are often a fraction of potential cyber losses, meaning that a single incident is not just a disruption. It can be an existential event.
At the same time, the Canadian Centre for Cyber Security says that ransomware remains a significant threat, and that extortion tactics will continue to intensify, particularly given cybercriminals' ability to use AI tools to accelerate and automate their attacks. For a clinic that depends on digital scheduling, imaging, billing, and patient records, that trend is not academic[1].
“A clinic does not buy cybersecurity to defend computers. It buys it to keep care, cash flow, and patient trust moving.” David Monroe, Awee CEO
Why the usual budget rules fail in a clinic
A clinic owner usually sees budget through categories such as payroll, supplies, rent, lab fees, and equipment. Cybersecurity hides inside IT management & support, software subscriptions, cloud backups, premium email licenses, consultancy services, privacy work, and staff training. Because it is fragmented, it is often underestimated.
The other reason clinics mis-budget cyber is that generic SMB ratios can be misleading at small scale. A 12-person clinic and a 200-person business both need secure identities, protected email, immutable backups, a documented recovery approach, and some form of detection and response. The smaller clinic cannot cut those categories to zero. This creates a floor cost below which the clinic is not truly protected, even if a spreadsheet suggests the spend is 'only' 8% of IT budget or 0.3% of revenue.
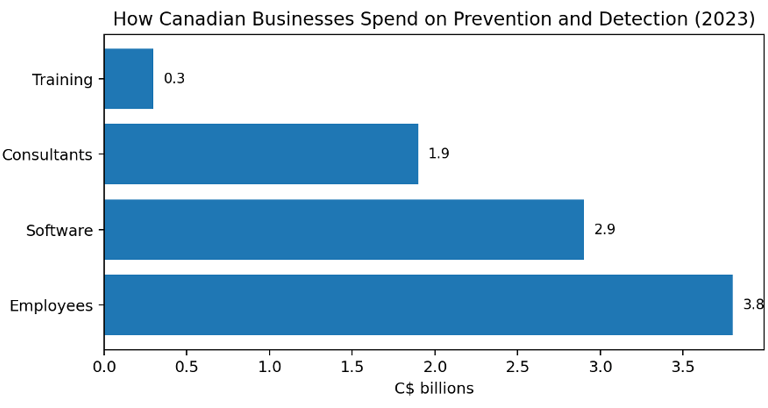
In fact, the official Canadian spending mix supports a broader view of the budget. Statistics Canada found that the largest category of prevention and detection cost in 2023 was employee salary related to security, followed by cybersecurity software and consultant or contractor expenses; employee training was smaller, but still material. The lesson is straightforward: cybersecurity is not a product line. It is a mix of people, software, outsourced expertise, and operating discipline[2].
Figure 1. Selected categories in Canadian prevention and detection spending, 2023
Values shown are selected line items explicitly reported in the release: employee salary related to prevention or detection ($3.8B), cybersecurity software ($2.9B), consultants/contractors ($1.9B), and training costs (over $0.3B).
Start with four lenses, not one
1. The threat lens: what would interruption cost this clinic?
Before debating tools, calculate the business consequence of disruption. Take annual collections or revenue and divide by the number of operating days to estimate production per day. Then add the downstream costs that do not show up on the appointment book: re-entry of data, overtime, forensic help, emergency IT work, communications with patients, legal advice, and management time.
If a clinic produces about $1.8 million a year over roughly 220 operating days, one disrupted day is already worth about $8,000 in production alone. A three-day interruption can therefore destroy $24,000 in gross production before recovery costs are counted.
2. The compliance lens: what information are you obliged to safeguard?
Dental clinics are not just ordinary small businesses. They hold personal and often highly sensitive health information. In Canada, federal and provincial privacy laws apply to private-sector organisations engaged in commercial activity. Depending on the province, substantially similar provincial private-sector or health-information statutes may also apply. The Office of the Privacy Commissioner stresses safeguards as one of the core principles. In budget terms, that means the clinic needs enough money allocated to identity protection, access control, backup, recovery, vendor discipline, and staff handling of information, not simply antivirus.
3. The market lens: what does protection actually cost in Canada right now?
For clinics that outsource most IT, market pricing gives a practical reality check. Canadian MSP pricing guides show managed IT commonly running around $100–$250 per user per month, while fully managed IT with advanced cybersecurity can run roughly $225–$400+ per user per month, with regulated sectors such as healthcare often paying more. Line-item pricing from Canadian providers also shows why the stack adds up: email security and backups can run about $10 per user per month; detection tools, like EDR, often adds roughly $3–$7 per endpoint per month; real time monitoring (SOC/MDR) can add $5–$20 per user per month; training and phishing testing add more. These are not official statistical benchmarks, but they are useful buying benchmarks.
4. The benchmark lens: how do you avoid false precision?
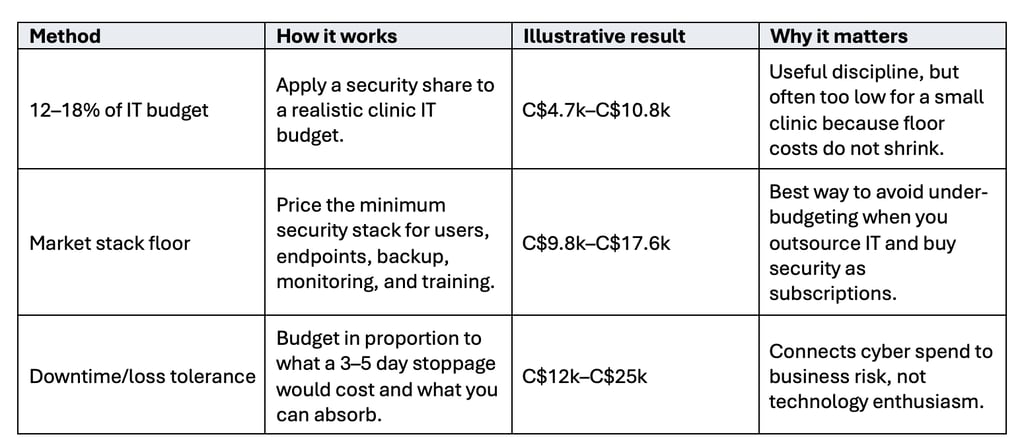
There is no single official Canadian benchmark that tells a dental clinic exactly how much cyber budget it should carry. The sensible answer is to triangulate. Use a share-of-IT benchmark for discipline; use headcount and endpoint-based buying benchmarks for realism; and use a business-impact estimate so the final number reflects what your clinic can actually afford to lose. This article therefore recommends taking the highest of three methods rather than trusting one tidy ratio. (Business.com, 2026).
A worked example: a 12-person clinic
Consider a clinic with 12 staff, 6 operatories, about 18 endpoints and shared devices, cloud email, a practice-management platform, digital imaging, and annual revenue of roughly C$1.8 million. The clinic is not a hospital; it is small enough that owner time matters and fixed costs bite. That makes budgeting discipline essential.
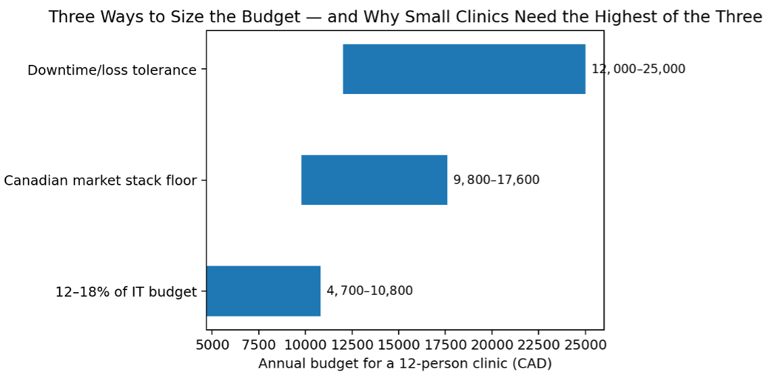
To size the annual cyber budget, compare three methods.
Decision assumptions used in this example: IT budget estimated from common Canadian managed-service pricing and ordinary software/support needs; market stack floor assembled from Canadian pricing references for email security/backup, EDR, monitoring, and awareness; downtime/loss tolerance based on a three-day interruption plus recovery effort. Because small clinics face non-shrinking fixed security costs, the decision should usually start from the highest of the three methods, not the lowest.
A realistic planning conclusion for this clinic is not C$5,000; it is closer to C$12,000–C$18,000 annually. This range is large enough to fund the minimum viable stack without pretending the clinic can build an enterprise-grade security team. It is also small enough to be phased over a year.
What the budget should actually buy
The point of the budget is not to buy “more security”. It is to reduce the specific ways a clinic fails under stress: stolen credentials, email compromise, ransomware on endpoints, failed restores, fraud, weak vendor controls, and staff mistakes. That requires a mix of controls.
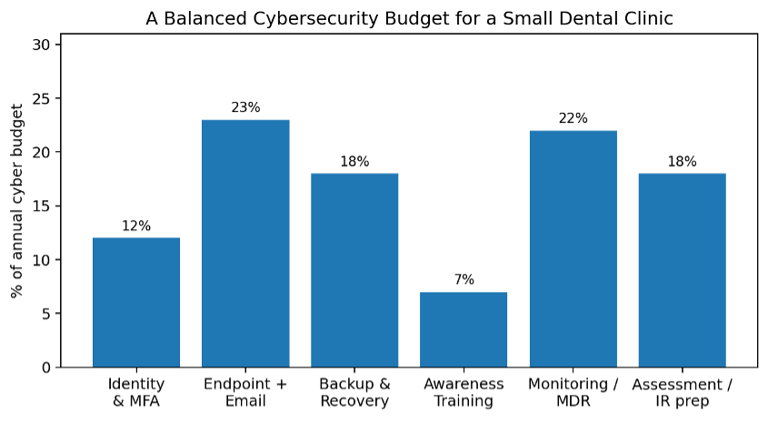
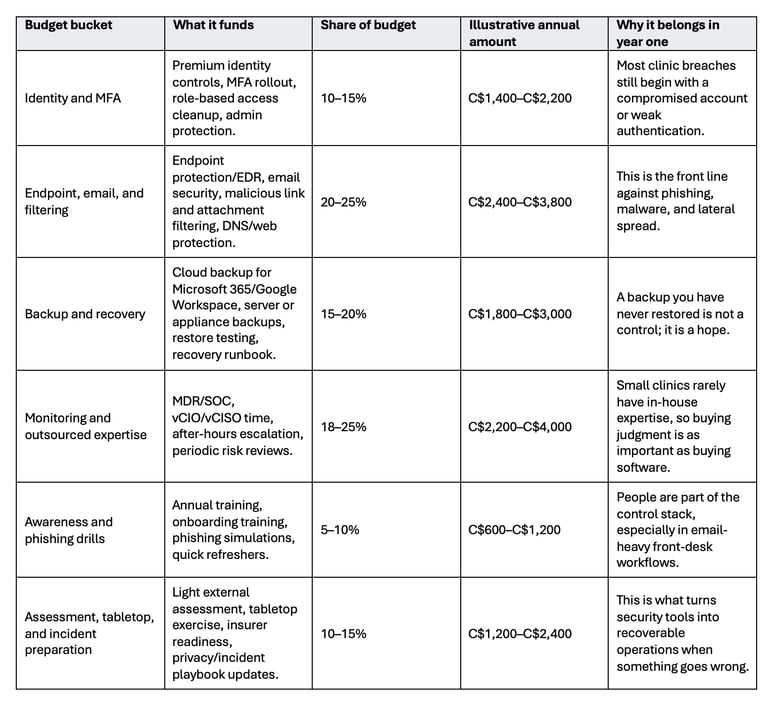
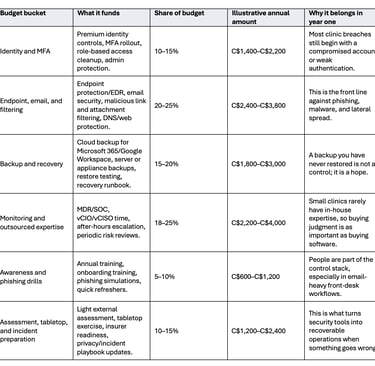
Recommended mix for a small clinic budget (12 employees). Exact percentages will vary, but the balance matters: too much software with too little recovery planning or training is a common failure mode.
A case vignette: what under-budgeting looks like in practice
Picture a clinic that has antivirus, but no tested backups, weak MFA coverage, no meaningful phishing drills, and no one clearly responsible for the incident response checklist. A staff member clicks a convincing radiography email. The attacker uses the account to push malicious messages internally and reaches a workstation used for scheduling and document exchange. The criminals exfiltrate all the data before encrypting it.
Even if the clinic never pays a ransom, the practical damage compounds quickly: lost production, manual rescheduling, patient communications, recovery labour, legal, forensics and external IT support, and management distraction. The clinic does not merely suffer a “cyber incident”; it suffers a week of poor operations, employee stress, systems and data recovery, reputational damages, potential fines or legal actions.
This is why the cheapest budget is often the most expensive one. Spending C$12,000 to C$18,000 a year can feel discretionary until you compare it with several days of lost production and a chaotic recovery. The budget should be judged against avoided interruption, not against the price of software alone.
A practical budgeting recipe for a clinic owner
Step 1: Identify the systems that stop care when unavailable.
List the handful of things without which the clinic cannot function for more than a few hours: scheduling, patient charts, digital imaging, billing/claims, email, access cards and internet/telephony. This becomes your budgeting anchor. If a control does not protect one of these, it is not year-one spending.
Step 2: Put a price on one day of disruption.
Use annual production divided by operating days, then add a rough allowance for overtime, legal fees, forensics and emergency IT labour, and patient communications. Owners often discover that one bad day costs more than several months of preventive subscriptions.
Step 3: Count users, endpoints, and privileged accounts.
Do not budget from headcount alone. Count shared devices, front-desk workstations, laptops, imaging stations, mobile devices with mail access, and any admin accounts. Many clinics under-budget because they price for users but forget the devices and identities that need protection.
Step 4: Fund the minimum viable stack before buying extras.
The first money should go to MFA, email security, endpoint protection, tested backups, awareness training and monitoring. Penetration testing or niche tools can wait if the basics are incomplete.
Step 5: Choose where to outsource judgment.
A small clinic should not try to buy only tools and manage them alone. Budget for at least some outside expertise, like a capable Managed Cybersecurity provider and security advisor, because the challenge in a real incident is not detecting every alert; it is making good decisions quickly.
Step 6: Phase the budget over 12 months.
Spread the work. Build a roadmap with your trusted partners: insurer, legal, cybersecurity and IT advisors. Prioritize basic controls over advanced ones to obtain a fast ROI.
Step 7: Review five board-style metrics every quarter.
Even a small clinic can track a handful of meaningful metrics: Human risk score (training performance), MFA coverage, immutable backup deployed and tested, monitored endpoints and systems. These cover the most critical controls that a small clinic should implement.
What not to do
· Do not report cyber to leadership as a technology line item only. Report it as reduced downtime and reduced privacy exposure.
· Do not define the budget as “whatever is left after equipment and payroll”. Basic routine is key to preventing major issues over time, just like in healthcare.
· Do not buy overlapping tools before you put in place basic controls, awareness, backups, MFA, and endpoint protection and monitoring are consistently in place.
· Do not rely only on your IT provider as your only strategy; ask for independent cybersecurity advice.
· Do not assume cyber insurance replaces the budget. Insurance is a financing mechanism; controls are what make you insurable and recoverable.
The real argument for the budget
A clinic owner does not need to become a cybersecurity expert to budget for it properly. What they do need is a better framework. The right question is not, "What is the perfect cybersecurity system?" Rather, it should be, "What is the smallest annual investment that meaningfully reduces the likelihood that my clinic will stop serving patients, become a victim of fraud, or mishandle patient information?"
That framing also explains why some widely quoted benchmarks should be used carefully. A global benchmark such as 13.2% of IT budget is a useful reference point, but it should be a floor discipline, not a ceiling. In small, compliance-sensitive environments such as dental clinics, the economics of security are shaped by fixed minimum controls and by the cost of interruption. The clinic should therefore treat cybersecurity as a resilience budget: partly IT, partly operations, partly privacy, and partly management insurance.
Done well, the budget becomes understandable. It is no longer a mysterious collection of subscriptions. It is a deliberate choice to preserve production, protect patient trust, prevent fraud and keep the clinic functioning when an attack or error occurs.
References
Baker Donelson. (2025). Cybersecurity awareness month: Avoid cyber claims scares (NetDiligence 2025 insights). Baker, Donelson, Bearman, Caldwell & Berkowitz, PC. https://www.bakerdonelson.com/cybersecurity-awareness-month-2025-avoid-cyber-claims-scares
Business.com. (2026, January 26). How much should your SMB budget for cybersecurity? https://www.business.com/articles/smb-budget-for-cybersecurity/
Canada Computing. (n.d.). Managed IT. https://canadacomputing.ca/mit/
Canadian Centre for Cyber Security. (2024, October 30). National Cyber Threat Assessment 2025–2026. https://www.cyber.gc.ca/en/guidance/national-cyber-threat-assessment-2025-2026
Canadian Federation of Independent Business. (2025). Digital transformation: How small businesses in Canada are leveraging AI and technology for growth and productivity. https://www.cfib-fcei.ca/hubfs/research/reports/2025/SMEs%20Digital%20transformation%20journey%202025-EN.pdf
Dentx. (2026, January 26). Dental overhead rate: Solo vs group practice. https://dentx.ca/blog/dental-overhead-benchmarks/
F12.net. (2025, April 28). 2025 managed IT services pricing guide for Canadian companies. https://f12.net/blog/2025-managed-it-services-pricing-guide-for-canadian-companies/
Happier IT. (2025). Managed IT pricing in Ontario & Western Canada (2025). https://www.happierit.com/insights-managed-it/insights-managed-it-managed-it-pricing-canada-2025/
IBM. (2025). Cost of a data breach report 2025. https://www.ibm.com/reports/data-breach
Insurance Bureau of Canada. (2025, October 1). Canadian small businesses are underprepared for cyber attacks, survey shows. https://www.ibc.ca/news-insights/news/canadian-small-businesses-are-underprepared-for-cyber-attacks-survey-shows
MoneyGeek. (2026). The cyber insolvency gap: Why small businesses are financially unprepared for cyber incidents. MoneyGeek. https://www.moneygeek.com/insurance/business/insolvency-gap/
NetDiligence. (2025). Cyber claims study 2025 report. NetDiligence. https://netdiligence.com/cyber-claims-study-2025-report/
Office of the Privacy Commissioner of Canada. (2024, May 1). PIPEDA requirements in brief. https://www.priv.gc.ca/en/privacy-topics/privacy-laws-in-canada/the-personal-information-protection-and-electronic-documents-act-pipeda/pipeda_brief/
Scott Insurance. (2025). Cyber risk trends and insights for small and mid-sized businesses. Scott Insurance. https://www.scottins.com/blog/cyber-risk-trends/
Sirkit. (2025, May 14). Comparing managed service provider: Price vs. value. https://www.sirkit.ca/blog/comparing-msp-offers-price-vs-value
Statistics Canada. (2024, October 21). Impact of cybercrime on Canadian businesses, 2023. The Daily. https://www150.statcan.gc.ca/n1/daily-quotidien/241021/dq241021a-eng.htm
[1] Statistics Canada, 2024; Canadian Centre for Cyber Security, 2024
[2] Source: Statistics Canada, The Daily, “Impact of cybercrime on Canadian businesses, 2023.”
Let's Connect
Transforming cybersecurity awareness into engaging experiences.
Contact us
© 2025. All rights reserved.
